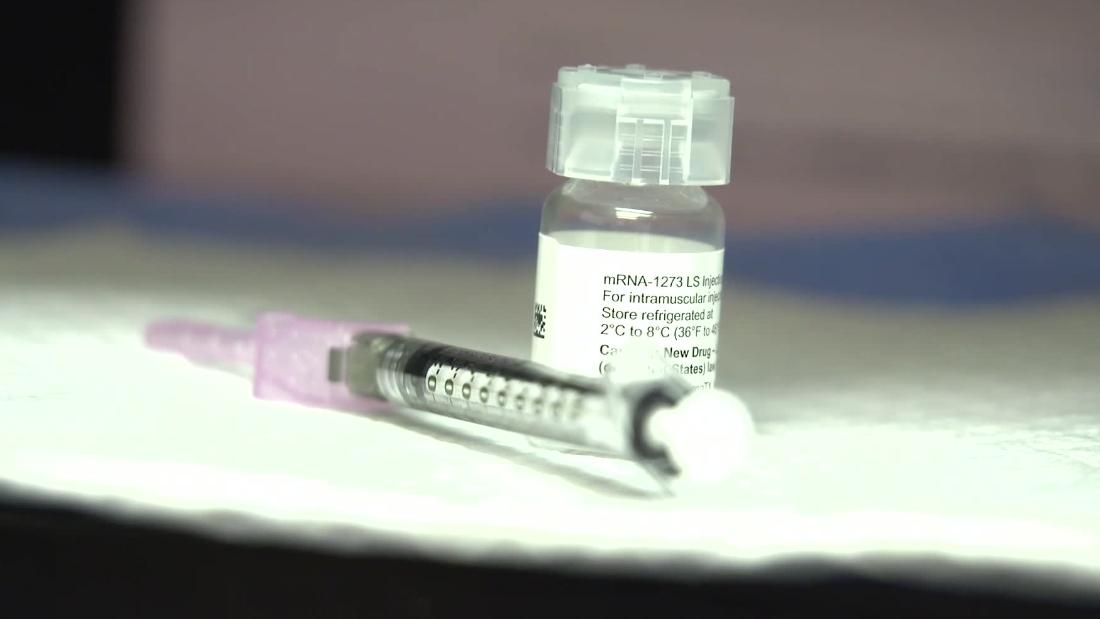
Vaccines like to be kept cool, none more so than the Pfizer candidate for Covid-19, which has to be deep-frozen. And that’s going to be an issue for developing countries — and for rural areas in the developed world.
The “cold rain” is just one of the challenges in distributing vaccines worldwide.
There are plenty of others: decisions about priority populations and databases to keep track of who’s received what vaccine, where and when. Additionally, different vaccines may have more or less efficacy with different population groups; and governments will need PR campaigns to persuade people that vaccines are safe.
But the logistics of transporting and storing vaccines– getting them from the factory gate to the patient’s arm– are critical. And as most vaccines are likely to require two doses, the whole chain needs must be repeated within weeks.
Unique challenges
The Pfizer-BioNTech vaccine needs to be kept at around -70 degrees Celsius (-94 degrees Fahrenheit) while it’s transported. That’s 50 degrees Celsius colder than any other vaccine currently used.
Moderna says its vaccine can be kept in freezers typically available in pharmacies, and in a refrigerator for up to 30 days. But there are likely to be fewer doses of the Moderna vaccine than of the Pfizer’s available over the next year.
Phase 3 trials have shown both vaccines to be around 95% effective but the results haven’t yet been reviewed by regulators.
On Wednesday, the CEO of BioNTech, the German biotech company partnering with Pfizer, acknowledged the issue of temperature control.

Employees fill a clinical and pharmaceutical product shipping box with dry ice at the Va-Q-Tec AG factory in Wurzburg, Germany, on Wednesday, Nov. 18, 2020.
“We are working on formulation which could allow us to ship the vaccine even maybe at room temperature,” Ugur Sahin told CNN. “We believe that in the second half of 2021 we will have come up with a formulation which is comparable to any other type of vaccine.”
But in the meantime US Health and Human Services Secretary Alex Azar believes the Moderna candidate is “more flexible” for settings like a local pharmacist. Pfiszer’s, he said Monday, would be better suited to “big institutional vaccination, say a while hospital setting, several nursing homes at once.”
Compare Medicare Plans Now
Pfizer plans to ship up to 1.3 billion doses next year, requiring a lot of dry ice (carbon dioxide in solic form at around -78 degrees Celsius), and a lot of isothermic boxes. The boxes will hold up to 95 vials (4,875 doses) and be refilled with dry ice for up to 15 days of storage.
Pfizer is testing the supply chain in four US states. Its CEO, Albert Bourla, said Wednesday he has “zero concerns” about the cold chain requirements.
But shipping such a vaccine can pose big challenges. Dr. Jarbas Barbosa, assistant director of the Pan American Health Organization, told CNN that “the rural and the urban areas in any country in the world are not ready to manage this vaccine today.”
“So, who is prepared in the world? No one.”
One issuee is the availability of dry ice.
The Compressed Gas Association says carbon dioxide production capacity in the US and Canada is about 30,000 tons a day and is confident its members can meet demand for dry ice. It says that vaccine supply-chain officials believe less than 5% of dry ice production will be needed to support ultra-cold storage of Covid-19 vaccines in the United States and Canada.
Others in the industry expect bottlenecks. Several dry ice producers in the US told CNN they’ve already had offers for their entire output. Buddy Collen at Reliant and Pacific Dry Ice told online publication GasWorld: “We are in scramble mode trying to manipulate our production plants.”
Sam Rushing, president of Florida-based Advanced Cryogenics, told CNN there are already regional shortages in the US.
The main problem, Rushing says, is fewer vehicles on the road during the pandemic, meaning lower production of ethanol, from which carbon dioxide is a byproduct. European ethanol production has also fallen sharply this year.
US officials are confident enough dry ice will be available. Paul Ostrowski, director of supply, production, and distribution of Operation Warp Speed, told CNN last week that courier UPS had pledged to “provide dry ice replenishments throughout all of America upon demand.”
But Rushing cautions that dry ice is not very user-friendly and can be hazardous if stored improperly, especially in a confined space. The Federal Aviation Administration classifies it as hazardous cargo.
Compare Medicare Plans Now
Peter Gerber, CEO of Lufthansa Cargo, told CNN that the need for dry ice “clearly reduces also the transport capacity because if you have to load more ice you can’t load so much vaccine. And of course the procedures have to be very special in order to ensure that it always has this degree of coldness.”
US courier DHL is adapting distribution plans according to each vaccine’s specifications. David Goldberg, CEO of Global Forwarding US for the company, says “there is a restriction on the amount of dry ice used on an aircraft– typically 500-1,000 kilos depending on a number of factors.”
Once they arrive, Pfizer vials can be stored at between 2 and 8 degrees Celsius for up to five days before deteriorating. Pfizer says it has developed a “just-in-time system which will ship the frozen vials direct to the point of vaccination.” It will also monitor the temperature of every box being shipped.
Julie Swann, an expert in supply chains at North Carolina State University, says that large hospital systems, which often have ultra-cool freezers, may have a role as distribution hubs. But not all US states have them; Hawaii said last week none of its hospitals has such freezers.
Breaking down shipments of a frozen vaccine for rural areas or small groups of essential workers– without compromising their temperature– will be another headache, Swann said.
When a vaccine needs to be used with a few days, providers will need to ensure they are ready. “You can’t just wait to see who shows up,” Swann told CNN. “And we don’t really have good data yet defining where and who the priority populations are.”
The more links in the supply chain, the more risk that the vaccine’s temperature will be compromised. Last month the US Centers for Disease Control and Prevention advised states they should “limit transport of frozen of ultra-cold vaccine products.”
Prashant Yadav, a supply chain expert and senior fellow at the Center for Global Development said: “It’s a question of how soon can we start thinking about multiple packaging formats.”
Beyond the US
If getting a frozen vaccine to tens of millions of people is a challenge in the US, it’s a far greater problem for poorer countries.
Transport links are slower and medical facilities less equipped in the developing world. CO2 production is scarce, and the cost and hazards of shipping huge amounts of dry ice are also a hurdle, Yadav says.
David Gitlin, the CEO of refrigeration specialists Carrier, told CNN last week: “When you look at places like Africa and India, they just don’t have the cold chain infrastructure. The Untied State spends 300 times more per capita on cold chain than India.”
Compare Medicare Plans Now
Peru is one of many countries that have order the Pfizer vaccine. In the capital, Lime, where large volumes can be administered quickly, it should be effective, says Dr. German Malaga, one of a team working on Peru’s vaccine options. But while there are probably 30 ultra-cold freezers in Lima “for the other 20 million Peruvians including in the Andes and the rainforest there are none.”
“For the rest of the country we could use vaccines like the Chinese one that requires from 2 to 8 degrees is more manageable,” Malaga said.
“It’s about cost-effectiveness, which is not just about the vaccine but the whole process of vaccinating,” said Yadav. But if Pfizer’s candidates proves to be the most effective, demand for ultra-cold freezers would be overwhelming.
Barbosa says the Pan American Health Organization is urging member states not to spend huge sums on preparing for one vaccine but join a multilateral facility called COVAX– essentially a clearing house for buying vaccines run by the World Health Organization.
Beyond the cold chain, there are other logistical hurdles.
A massive airlift will be required to get vaccines where they need to go. Pfizer, which has production lines in Europe and the US, says it expects an average of 20 daily cargo flights worldwide.
DHL expects that 15 million cooling boxes will need to be delivered on 15,000 flights over the next two years. David Goldberg told CNN the company has established a high quality cold-chain network and is adding flights between China, Europe and the US.
Compare Medicare Plans Now
Many countries can call on existing programs as models. Peru’s national vaccination program reaches about 75% of its population, Malaga said.
India’s polo vaccination program is ubiquitous– covering more than 90% of children by this year, according to Gagandeep Kang of the Wellcome Trust Research Laboratory at the Christian Medical College in Vellore.
“For polio programs, we have used boats and mules and enterprising health staff,” said Kang. But such programs are designed for less than a tenth of the population, and Covid-19 vaccines will need to focus on different groups, she said.
India will need “a series of waves each addressing a different group as vaccines become available,” she told CNN.
“We will need to see performance characteristics of other vaccines, and their delivery requirements before making a call on what to go with,” said Kang, who is also a member of the World Health Organization’s Global Advisory Committee on Vaccine Safety.
In such a dynamic situation, record-keeping becomes critical. Dr. Anna Blakney, who is working on a vaccine being developed by Imperial College London, said there is no centralized infrastructure in the US for monitoring who is getting what and when, which she describes as a “really critical issue.”
Yadav says that even when the vaccine reaches its destination there will need to be some flexibility to allow people to get their second dose in a different location if desired. And that demands reliable databases.
Barbosa said that beyond the supply chain, governments “must have a good communications strategy to overcome public skepticism and conspiracy theories about vaccines.”
Blakney agrees. “The process [of vaccine development] has been so fast that it’s not surprising people are skeptical as they read about safety and possible side-effects,” she said. Blakney is part of an international effort launched by research scientists to reassure people via social media about the safety and efficacy of Covid-19 vaccines.
Finding enough dry ice is just one in a sequence of challenges to get the world vaccinated against Covid-19.
Read More…
Powered by NewsAPI.org
Compare Medicare Plans Now